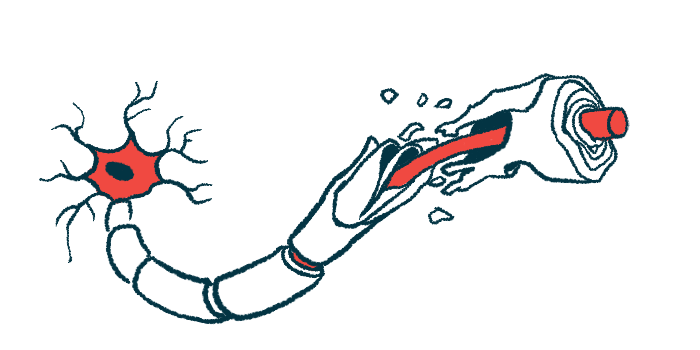
Guillain-Barré Syndrome is a rare autoimmune disorder where the immune system attacks peripheral nerves. It often occurs after infections and leads to sudden muscle weakness, starting in the legs and potentially spreading upward.
Patients may experience tingling, numbness, difficulty walking, and in severe cases, paralysis or breathing difficulties requiring intensive care. Reflexes are often reduced or absent. Though frightening, many patients recover fully with timely treatment.
Diagnosis involves clinical exam, nerve conduction studies, and lumbar puncture. Treatment includes intravenous immunoglobulin (IVIG) or plasmapheresis. Supportive care and rehabilitation are essential for recovery.

CIDP is a chronic autoimmune disease in which the immune system attacks the myelin sheath of peripheral nerves, leading to progressive weakness, numbness, and impaired reflexes in the arms and legs. It is considered the chronic counterpart of Guillain-Barré Syndrome.
Symptoms usually develop slowly over weeks or months and may include difficulty walking, climbing stairs, or lifting objects. Unlike GBS, CIDP progresses gradually and can relapse over time if untreated.
Diagnosis is confirmed through nerve conduction studies, EMG, and spinal fluid analysis. Treatment includes corticosteroids, IVIG, or plasmapheresis, and long-term immunosuppressive therapy may be needed in some cases.
Myasthenia Gravis is a chronic autoimmune disorder in which antibodies block or destroy acetylcholine receptors at the neuromuscular junction, preventing proper muscle contraction. This leads to weakness in voluntary muscles, especially after activity.
Common symptoms include drooping eyelids (ptosis), double vision, difficulty speaking, swallowing, and generalized fatigue. Symptoms often worsen with exertion and improve with rest.
Diagnosis involves antibody testing, electromyography (EMG), and response to medications like neostigmine. Treatment includes acetylcholinesterase inhibitors, corticosteroids, immunosuppressants, and in some cases, thymectomy or plasmapheresis during crises.
MMN is a chronic autoimmune condition that selectively affects motor nerves, leading to slowly progressive weakness, typically in the arms and hands. Unlike other neuropathies, MMN does not involve sensory nerves, and reflexes are usually reduced in affected limbs.
Symptoms include asymmetrical limb weakness, muscle twitching (fasciculations), and muscle wasting. It can mimic conditions like ALS, but MMN is treatable and non-fatal.
Diagnosis is based on clinical findings, nerve conduction studies showing conduction block, and the presence of anti-GM1 antibodies. Treatment typically includes intravenous immunoglobulin (IVIG), which often leads to noticeable improvement.

Nodopathies are a group of autoimmune neuropathies where the immune system attacks the nodal or paranodal regions of peripheral nerves, disrupting signal conduction without classical demyelination. These are distinct from typical demyelinating conditions.
Symptoms may include rapid-onset or progressive limb weakness, reduced or absent reflexes, and sometimes sensory changes. Some patients experience overlap with Guillain-Barré Syndrome variants but respond differently to treatment.
Diagnosis involves detecting specific antibodies (e.g., anti-CNTN1, anti-NF155, anti-Caspr1), supported by nerve conduction studies. Treatment includes IVIG, steroids, or rituximab depending on antibody subtype and response.
Neuromyotonias, also known as Isaacs’ syndrome, are rare disorders characterized by continuous muscle fiber activity due to hyperexcitability of peripheral motor nerves. These conditions are often autoimmune in nature and may be associated with antibodies like CASPR2 or LGI1.
Symptoms include muscle stiffness, cramps, twitching (fasciculations), delayed relaxation, and excessive sweating. Symptoms often persist during rest and may worsen at night, leading to sleep disturbances.
Diagnosis is confirmed through electromyography (EMG), antibody testing, and clinical evaluation. Treatment may include anticonvulsants (e.g., phenytoin, carbamazepine), immunotherapy, and plasma exchange in antibody-positive cases.